Addressing substance use requires a comprehensive approach involving prevention, treatment, and recovery support services.
At HCPSC, there are healthcare professionals who offer inpatient and outpatient counseling, treatments, and medication-assisted therapy for substance use.
Here are a few options you can avail in the context of substance use by registering with HCPSC.
Cognitive and Behavioral Therapies
Cognitive behavioral therapy or CBT techniques are now widely used to treat substance use disorders. These techniques are not only effective for the treatment of unhealthy use of drugs, but also target other behavioral health disorders, such as OCD, eating disorders, bipolar disorder, and anxiety.
There are qualified behavioral therapists at HCPSC who help their patients understand that they need to get rid of automatic negative thoughts that lead to depression, anxiety, and ultimately substance use as a coping mechanism.
These approaches emphasize the importance of developing coping skills to manage triggers and stressors that may lead to relapse.
At HCPSC, SUD patients are provided with self-help tools so they can divert their negative thoughts to something that makes them happy. Therapists also make sure that patients are able to overcome their insecurities and false beliefs that lead to substance abuse.
Medication-Assisted Therapy
MAT or medication-assisted treatments are available for drug use disorders, including alcohol, tobacco, and opioids use disorder. In this type of therapy, certain medications are used in conjunction with other techniques to provide relief to patients when they are experiencing withdrawal symptoms.
The medications used in MAT help reduce cravings and withdrawal symptoms, making it easier for individuals to focus on their recovery. Along with medication, counseling and support groups help individuals develop healthy coping mechanisms and skills to prevent relapse.

It has been observed that MAT can be used for months or even years for as long as it’s needed. The medications used in the treatment have no serious adverse effects and they have not been found to affect a person’s intelligence or mental capability.
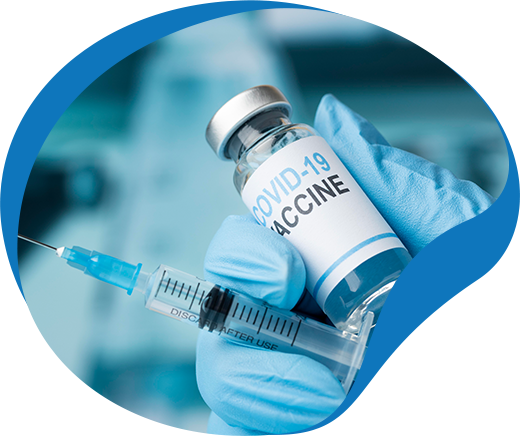
COVID-19 Vaccination for People with Substance Use Disorders
People impacted by SUDs sometimes show unwillingness to receive any type of vaccine. Some of them show feelings of uncertainty, while others show readiness but after a delay.
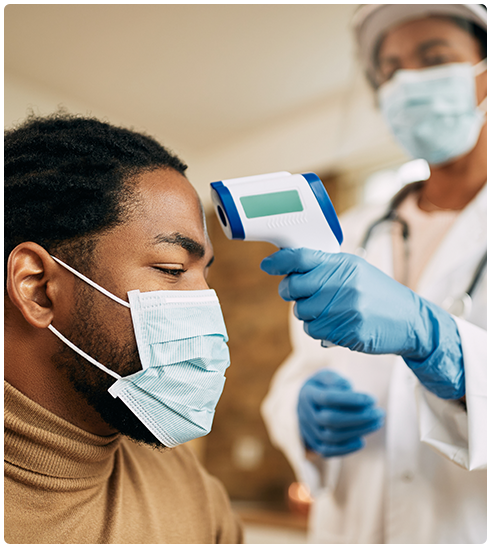
Since these people are at a higher risk of catching the COVID-19 infection and developing complications later on, in order to mitigate this risk, it is vital for healthcare professionals to ensure that they trust the vaccine and are ready to receive it.
At HCPSC, special training has been given to healthcare professionals in this regard. They take proper steps to ensure that substance use patients are completely willing to get vaccinated against COVID-19.
Substance Use & COVID-19
Substance use is a behavioral disorder that needs to be addressed in the context of COVID-19 since it is one of the major contributors to poor behavioral and emotional health during the pandemic.
The stress and anxiety caused by the pandemic have led to an increase in substance use, particularly among vulnerable populations.
This disorder affects a person’s behavior as they feel unable to control their use of substances, including certain legal and illegal drugs.
A person will be diagnosed with substance use disorder or SUD if he or she is unable to control the use of;
Some people also include alcohol, stimulants like tobacco, and prescription drugs to this list. However, the above-mentioned substances fall under the category of internationally controlled substances (drugs).
So, the term “drug use disorders” refers to the non-medical use of the above-mentioned drugs. And the term “substance use disorders” covers non-medical use of drugs mentioned above as well as alcohol, tobacco, and prescription drugs.
Substance use disorders have become a significant cause for concern in the United States.
According to a recent survey, more than 40 million Americans have suffered from a substance use disorder at some point in their lives.
It is important to recognize the seriousness of this issue and to provide support and resources for those who are struggling with substance use disorder.

Psychiatric Disorders and Substance Use
Psychiatric disorders like;
- Depression,
- Anxiety
- Self-harm, and
- Suicidal ideation
are highly prevalent among people with substance use disorders [7].
These conditions even worsen when there is loneliness, self-isolation, and financial stress.
Individuals with behavioral health issues use drugs or alcohol as a form of self-medication to alleviate their symptoms. Unfortunately, this can be risky and may result in further exacerbation of their emotional condition.
The COVID-19 pandemic has brought on a severe economic crisis all over the world. These circumstances have led to an even higher number of substance use cases.
Moreover, people now have limited access to substances due to the restrictions imposed by the governments. This situation leads to withdrawal symptoms, such as fever, fatigue, body aches, and chills, which are very much similar to COVID-19 symptoms.
Unfortunately, most people do not seek medical help for the resolution of these symptoms.
As a result, they go into a lapse or relapse.
How Are Substance Use Disorder and COVID-19 Related?
People with substance use disorders have a compromised immune system because the condition can harm their lung function.
These people also have one or many underlying health conditions, such as heart disease, diabetes, hepatitis, and HIV.
As such, people with substance use disorders may have both behavioral as well as physical health comorbidities or both [3]. Those who have another emotional health issue combined with SUD are said to have “dual disorders”.
People with dual disorders are more likely to experience hospitalization as a result of some health complication. Because of these reasons, substance use disorder patients may experience severe symptoms and complications if they get COVID-19 [1].
It is recommended that people with SUD always maintain contact with their healthcare provider, especially during the pandemic.
They should immediately call their doctor if they experience one or more typical symptoms of COVID-19, such as fever, cough, loss of smell and taste, and sore throat.
It is important to remember if you have a SUD, your condition can be much more severe than other people’s when you contract the virus, and therefore it’s important to seek medical help.
Recent studies have shown that individuals who have been diagnosed with substance use disorder are also at a higher risk of contracting COVID-19.
Additionally, drug use often involves close contact with others, such as sharing needles or engaging in risky behaviors, which can increase the risk of exposure to the virus.
Moreover, a study has revealed that people who have been recently diagnosed (within the past year) with a SUD are 8 times more likely to contract COVID-19 than those who have a lifetime SUD [8].
The same study has found out that individuals with opioid use disorder and African Americans with a substance use disorder (SUD) have a higher likelihood of being hospitalized after contracting the infection.
It was found that severe outcomes of COVID-19 in these patients is also due to another underlying condition, such as diabetes and hypertension.
The likelihood of getting the infection also increases when these people ignore social distancing measures when they try to acquire illicit drugs. This is because drug deals often happen in close proximity, which puts both the buyer and the seller at risk of contracting the virus
An Increase in Substance Use Cases After COVID-19
Research has confirmed that substance use and drug overdose cases have seen a rise since the onset of the pandemic [4].
This is primarily due to increased emotional distress following the pandemic that has led people to rely on maladaptive coping mechanisms. And one of these mechanisms is excessive use of alcohol and drugs [6]
For individuals who are already struggling with substance abuse, the added stressors brought on by the pandemic can significantly increase the likelihood of relapse. Moreover, there has been a disruption in getting access to essential treatment and recovery programs, which has further exacerbated the situation.
been a disruption in getting access to essential treatment and recovery programs, which has further exacerbated the situation.
According to a study conducted in 2021, a 23% rise in alcohol abuse and 16% rise in drug abuse cases was observed since the beginning of COVID-19 in 2020 [5].

The pandemic has not only increased the likelihood of developing an SUD, but due to SUDs people are also at a higher risk of getting infected.
Since people with SUDs have compromised immune systems, in addition to COVID-19 and other viral infections, they are also highly vulnerable to;
- Upper respiratory infections,
- Cardiovascular complications, and
- Chronic obstructive pulmonary disease or COPD
In SUD patients, COVID-related complications can occur due to impaired respiratory function and inflammation response, both of which are a result of activation or depression of opioid receptors in the brain.
Studies show that there has been a higher prevalence of substance abuse among the Black and Hispanic populations since the pandemic [5].
Many of these individuals have reported starting or increasing substance abuse as a way to cope with various behavioral health issue
While substance abuse affects people of all races and ethnicities, the reasons for its prevalence among Black and Hispanic populations may be related to lack of access to behavioral health care services.
Risk Factors for COVID-19 If You Have SUD
SUD patients usually have different comorbidities that increase their risk of contracting the virus. We discuss here four of these risk factors.
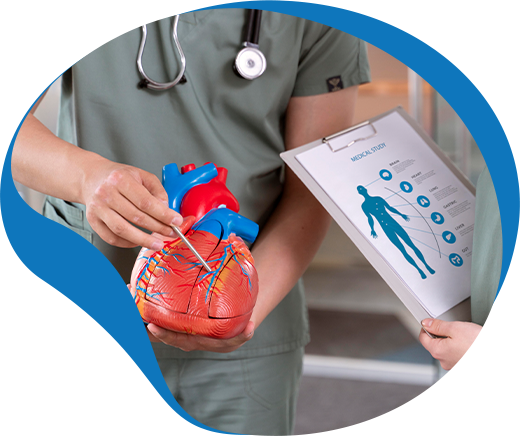
Cardiovascular
Individuals with substance use disorder are at an increased risk of developing a range of cardiovascular conditions.
Hypertension, or high blood pressure, is a common co-occurring condition, and can contribute to the development of more serious complications such as coronary heart disease or peripheral artery disease.
Other cardiovascular conditions such as arrhythmias, or irregular heartbeats, can also develop as a result of substance abuse.
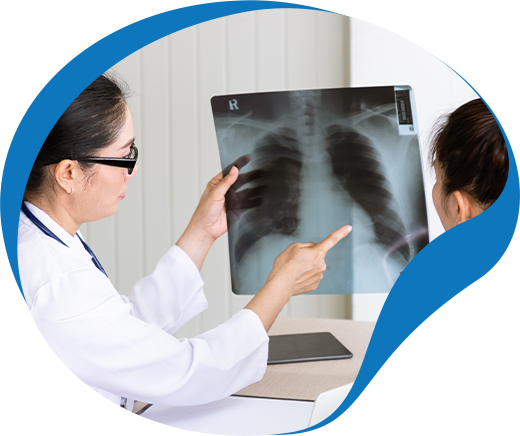
Pulmonary
Substance use patients often present with a variety of comorbidities, with pulmonary tuberculosis (TB), chronic respiratory disease, and asthma being among the most common.
These conditions can have a significant impact on the patient’s overall health and well-being, as well as their ability to seek and receive effective treatment for substance use disorders.
Metabolic diseases
Research has indicated that individuals with substance use disorders may have underlying metabolic diseases. Specifically, these individuals may be at an increased risk for conditions such as viral hepatitis, diabetes, and chronic kidney disease.
It’s important for healthcare providers to diagnose these conditions in substance use patients to suggest a viable treatment.

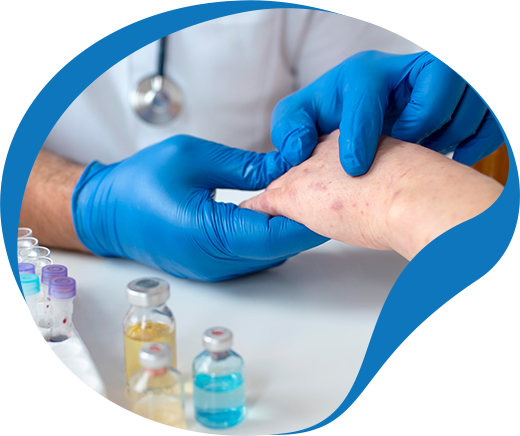
Increased sensitivity to infections
People with substance use disorders are more susceptible to opportunistic infections due to little or no access to proper healthcare, vaccination, and treatment. These infections (including COVID-19) may cause serious complications in these individuals if not controlled on time.
Social distancing measures and fear of infection have resulted in limited access to drug use disorder treatment services in the United States.
Many treatment facilities have had to limit their capacity or even shut down entirely due to concerns over the spread of COVID-19. This has made it difficult for individuals struggling with substance use disorder to access the help they need.
It was also found in a study published in 2020 that among the generalized population diagnosed with SUD, African Americans were more likely to get COVID-19 than Caucasians [2].
This is possible because African Americans who have substance use disorder have a higher prevalence of comorbidities, including diabetes, hypertension, asthma, obesity, and HIV, than Caucasians.
It is, therefore, crucial to prioritize the safety of individuals with substance use disorders, especially during this unprecedented time, and ensure that they have access to essential healthcare services.
COVID-19 Vaccine and Substance Use Disorder
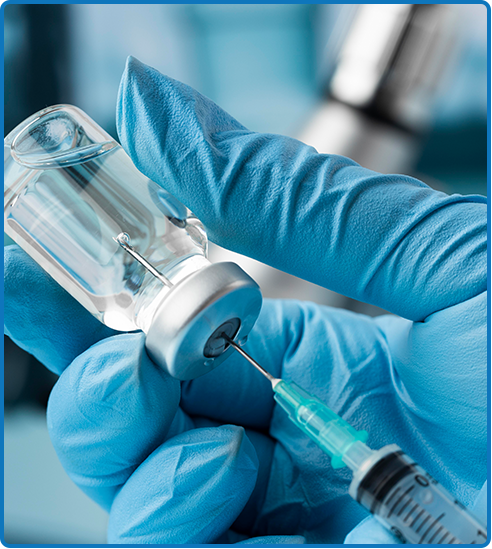
COVID-19 vaccines have been found to be perfectly safe for people with substance use disorders. In fact, it is recommended for these patients to receive a COVID-19 vaccination as soon as possible.
While there was initial concern about the potential impact of the vaccine on those with substance use disorders, research has shown that it does not impact the condition or recovery.
Moreover, individuals with substance use disorders are at a higher risk for developing severe complications from COVID-19, making the vaccine even more crucial for their health and well-being.
Substance use disorders are considered underlying medical health conditions – ones that can increase the risk of complications from COVID-19.
Even if someone is taking medications for opioid use disorders, such as methadone or buprenorphine, they can receive COVID-19 vaccination without experiencing any side effects [4].

